Life Over Limb
In high-energy trauma, survival governs decision-making.
Limb salvage is considered only after physiologic stability is secured and life-threatening injuries are addressed.
These decisions require disciplined assessment, not reflex intervention.
Salvage must serve the patient — not the procedure.
Judgment defines outcome.
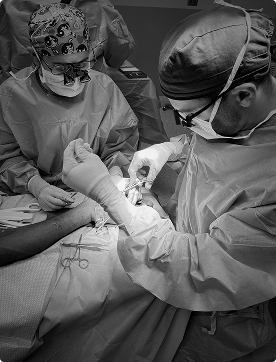
Traumatic Amputation & Extremity Threat
High-energy trauma may result in partial or complete traumatic amputation of the upper or lower extremity.
In select cases, replantation or revascularization remains possible.
These injuries demand immediate microsurgical capability embedded within trauma-scale infrastructure where vascular, orthopedic, and critical care coordination occur simultaneously.
Time-sensitive evaluation determines viability.
Replantation Capability
Advanced replantation and limb salvage require microsurgical capability integrated within trauma-scale infrastructure.
Replantation may include:
- Digit replantation
- Hand replantation
- Forearm or upper extremity revascularization
- Complex arterial and venous reconstruction
- Skeletal stabilization with coordinated soft tissue coverage
- Nerve repair with staged functional planning
Replantation is not a single procedure.
It is a structured sequence involving vascular restoration, skeletal stabilization, tendon reconstruction, nerve repair, and longitudinal rehabilitation.
Execution requires infrastructure capable of managing thrombosis risk, reperfusion injury, staged reconstruction, and intensive monitoring.
Limb Salvage Doctrine
Not all devastating extremity injuries are candidates for salvage.
Assessment incorporates:
- Ischemia time
- Degree of crush or avulsion
- Contamination burden
- Systemic injury severity
- Functional recovery potential
In borderline cases, coordinated consultation among trauma surgery, orthopedics, vascular surgery, and microsurgery determines whether salvage offers meaningful long-term utility.
When salvage is appropriate, it proceeds within a coordinated trauma framework.
When salvage compromises life or long-term function, amputation may represent the more appropriate intervention.
Measured judgment preserves safety and outcome integrity.
Functional Outcome Planning
Limb survival does not equal function.
Replantation and revascularization planning integrates:
- Nerve reconstruction
- Tendon restoration
- Soft tissue durability
- Rehabilitation sequencing
- Secondary revision planning
Functional recovery is structured from the initial operation forward.
The objective is meaningful use — strength, dexterity, sensation, coordinated motion.
Functional outcome after replantation is determined as much by structured rehabilitation as by the index operation.
Specialized Postoperative Hand Rehabilitation
Successful replantation and limb salvage extend beyond the operating room.
Postoperative rehabilitation is integral to outcome.
Highly specialized hand and upper extremity occupational therapy is coordinated through the rehabilitation hospital located on the grounds of the Level I trauma center.
Therapists experienced in replantation, tendon reconstruction, nerve repair, and free functional muscle transfer work in direct collaboration with the surgical team.
Therapy protocols align with operative sequencing, vascular monitoring, tendon glide preservation, and staged nerve recovery.
Early, structured rehabilitation is as critical to functional recovery as microsurgical reconstruction itself.
In complex extremity salvage, surgical precision and rehabilitation precision operate as a unified strategy.
Regional Tertiary Capability
Within Palm Beach County, advanced replantation and limb salvage are delivered within a Level I trauma infrastructure capable of immediate escalation.
The program evaluates referrals from across the county and a broader regional catchment area, including cases originating at other acute care and trauma facilities.
Inter-facility collaboration supports rapid tertiary evaluation when replantation, revascularization, or advanced salvage is under consideration.
Complex extremity injuries are frequently transferred for microsurgical assessment when higher-level reconstructive sequencing is required.
Immediate access to vascular support, staged operative capacity, and coordinated rehabilitation preserves viability and functional potential.
Escalation & Transfer
Time-sensitive extremity injuries require rapid evaluation.
Inter-facility and out-of-state transfer by air ambulance has been accepted in select cases where salvage potential exists.
Early consultation preserves reconstructive options.
Delay narrows them.
Professional Referral
Consultation may be requested for:
- Traumatic amputation
- Partial amputation
- Revascularization evaluation
- Failed salvage
- Secondary functional reconstruction
Inter-facility collaboration supports rapid tertiary evaluation when replantation, revascularization, or advanced salvage is under consideration.




